Meniscus rupture
A meniscus rupture means an injury to the cartilage discs in the knee joint (menisci). The menisci can be either torn or completely severed.
Learn more about meniscus rupture in this article: What exactly is a meniscus rupture and what are its symptoms? What causes a meniscus rupture? What are the possible treatments and therapies? And much more …
What is a meniscus rupture?
A meniscus rupture is an injury to the crescent-shaped and wedge-shaped cartilage discs of the knee joint. A meniscus can either be torn or severed due to external force, or may degenerate due to age or predisposition.
The menisci, which consist of an inner and outer meniscus, form the connection between the head of the tibia and the femoral condyle. Thanks to their crescent and wedge shape, they enable a smooth interaction between the differently shaped bony parts
of the knee joint.
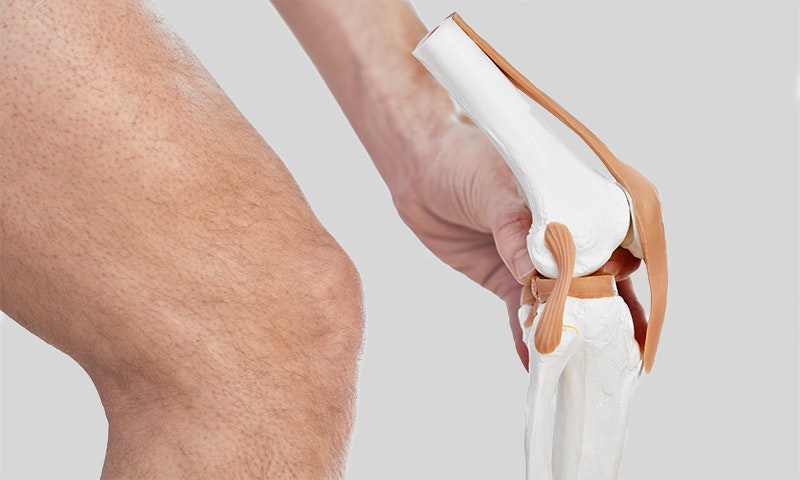
The cartilage discs, which are composed of one-third collagen and two-thirds water, act as shock absorbers, stabilisers, and load distributors in the knee joint.
The inner meniscus is firmly attached to the joint capsule of the knee. It is thus more frequently exposed to the damaging effects of external rotary movements than the more flexible outer meniscus. As a result, a meniscus rupture is more often a tear of the inner meniscus.
Meniscus ruptures are classified according to their orientation. Thus they can be classified in relation to the longitudinal axis or the horizontal plane.
In relation to the longitudinal axis:
- longitudinal tear
- horizontal tear
- radial tear
In relation to the horizontal plane:
- vertical tear
- horizontal tear
Meniscus ruptures are divided into 4 different degrees, depending on the severity of the injury. Degrees 1 and 2 can be treated conservatively. The tear has not yet penetrated the surface of the meniscus, and the damage can still be naturally
repaired. Degrees 3 and 4, on the other hand, require immediate surgical treatment. Subsequent rehabilitation to restore the function of the knee joint is also of great importance in this case.
From an epidemiological point of view, men are twice as likely to be affected by meniscus tears as women. Most tears occur to persons between the the ages of 30 and 50. Internal and external meniscus injuries occur in a ratio of 5:1 (Ruchholtz & Wirtz 2013).
Symptoms of meniscus rupture
The symptoms vary depending on whether the meniscus rupture is acute or caused by wear. A common symptom in both forms is a severe pain in the knee, especially under stress and during certain movements (e.g. due to entrapment of the meniscus in the case of unstable tears).
The acute (accident-related) meniscus rupture, for example, due to sports, causes a sudden and piercing pain in the knee joint and swelling.
A meniscus tear caused by wear develops gradually and manifests itself as increasing pain, which is often felt when the knee is under stress. This form of injury also causes a feeling of instability in the knee.
In general, a meniscus rupture manifests itself via the following symptoms:
- pain when bending, stretching, or turning the knee
- pain under stress
- swelling
- feeling of instability
- narrowing in the knee joint
- audible cracking or snapping noises
Narrowing of the knee joint occurs when a piece of cartilage loosens and gets stuck in the joint as a foreign body. This may cause painful movement and load limitations, which may lead to a complete blockage. It is then no longer possible to bend and
stretch the knee.
The symptoms vary depending on the cause of the meniscal tear. While acute tears cause sudden and piercing pain with swelling, wear-induced meniscus tears cause gradually increasing pain. This pain is felt particularly when the affected knee is under stress. Audible cracking noises and a feeling of instability also indicate an injury.
Suspected meniscus rupture - first aid
If a meniscus rupture is suspected, the affected knee should be raised, immobilised, and kept cool. Rest is the top priority!
Over-the-counter analgesics may help in the case of severe pain.
Diagnosis: meniscus rupture
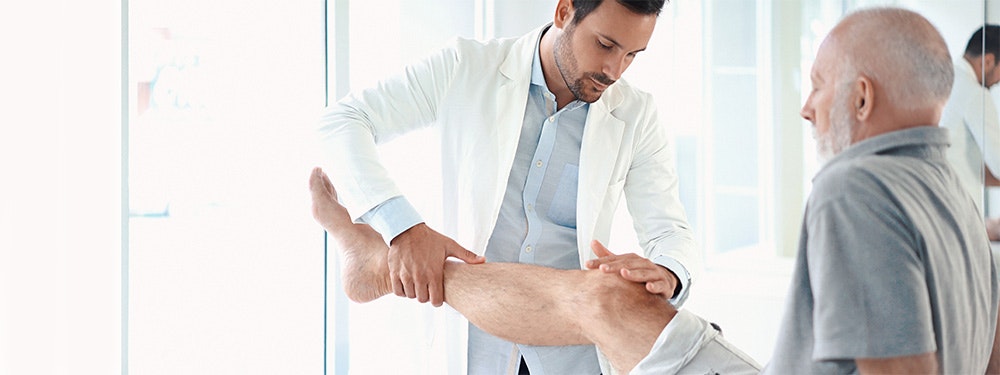
The initial assessment is made based on the patient’s medical history. The aim is to determine whether there is already a pre-existing medical condition or injury (such as a cruciate ligament rupture) which could be the reason for the pain. The patient is then subjected to a clinical examination. Provocation tests are used to test mobility and pain reactions via targeted manual manoeuvres by the physician. The following tests are performed:
- Steinmann test part I
The physician bends the patient's knee by 90 degrees and then turns their lower leg inwards and outwards. Pain in the inner knee (medial joint space) when the leg is turned outwards indicates an injury to the inner meniscus. On the other hand, pain when the leg is turned inwards indicates damage to the outer meniscus.
- Steinmann test part II
The physician presses on the meniscus while the patient's leg is stretched and bent. In an injury to the meniscus, there is a characteristic displacement of painful points towards the rear with increasing flexion.
- Bohler's sign
The patient extends the leg, and the physician adducts and abducts the patient's lower leg. There is increased pressure at the lateral joint space on abduction (when the foot moves outwards). If pain occurs on the side of the knee, this indicates damage to the outer meniscus. Due to the increased tension on the opposite medial joint space, this movement can also be used to test the medial (inner) collateral ligament. On the other hand, pain that is felt during the adduction movement (when the heel moves inwards) indicates damage to the inner meniscus or the lateral collateral ligament.
- Payr’s sign
The leg to be examined is brought into a cross-legged position (knee joint bent, hip joint abducted, foot above the knee of the other leg). In this position, the knee is then pressed towards the floor. If there is damage to the inner meniscus, pressing down causes pain inside the knee.
- Apley test
The patient lies on his or her stomach while the leg is bent by 90 degrees and the sole of the foot is pressed from above. The physician now rotates the patient's foot inwards and outwards. Depending on the direction of rotation, there is pain in the outer or inner meniscus if there is meniscal damage.
Imaging techniques can also be used to examine the condition of the menisci. X-rays can provide more information about the bony structures and will show wear damage. An MRI scan can also provide information that is relevant to the prognosis and the therapy by analysing factors such as the size, location, and structure of the tear (Waldt 2013).
An MRI scan is also highly recommended to rule out accompanying injuries, such as ligament tears in the knee.
Causes of a meniscus rupture
The most common cause of meniscus tears are accidents. In sports, in particular, overextending the knee in combination with a rotational movement and a sudden stop may cause injury to the menisci due to the excessive shear forces. This type of accident is seen especially in such sports as football, tennis, or skiing. Injuries to the menisci often occur in combination with torn ligaments. This is because the violent twisting and the abrupt stop also damages other structures in the knee joint (Becker et al. 2015).
Even lighter loads when running or in everyday life may, over the long term, strain the knee and the menisci (in the sense of repeated microtraumas). Regular overloading causes degeneration of the menisci and leads to subsequent meniscus tears. This effect is reinforced by obesity.
The regenerative capacity of the menisci decreases with increasing age. The cartilage discs become brittle and tear more easily. Many small tears then result in a complete meniscus rupture, even under light loads.
Risk factors for a meniscus rupture
The likelihood of a meniscus rupture is affected by genetic predispositions, such as the anatomical variant of discoid meniscus where the meniscus is round rather than sickle-shaped and may thus cause a pathological load distribution and discomfort. Misaligned legs, such as knock knees (genu valgum) or bow legs (genu varum), can also have a negative effect on the cartilaginous discs in the knee joint, and may accelerate wear.
Cruciate ligament ruptures make the knee more unstable, which greatly increases the load on the menisci.
Follow-up after a meniscus rupture
The treatment time, and the success of treatment, depend on the type, size, and the exact location of the meniscus rupture, and the age of the patient. If the tear is located near the fused section of the joint capsule, the chances of recovery are good due to the increased blood flow in that location.
In principle, acute, injury-related meniscal tears have a higher chance of healing than degenerative or wear-related tears. For younger patients, permanent knee pain, blockages in the knee, and injuries in the inner area of the meniscus are operated on relatively quickly and have a good chance of recovery. This also applies to traumatic injuries.
Degree 1 and 2 tears are usually treated conservatively (without surgery). Surgery is usually required from degree 3. Like all interventions, this procedure involves certain risks.
Surgeries in this area are performed arthroscopically (minimally invasive) through two small incisions on both sides of the knee. Depending on the case, the procedure involves a meniscus suture or a partial removal (resection).
Injury-related meniscal tears have a higher chance of healing than degenerative tears. Surgery for a meniscus tear is usually performed quickly, especially for younger patients. The chances of recovery are very good.
How long will I be on sick leave?
A partial meniscus removal only requires a hospital stay of approx. 2 to 3 days, and a relatively short period of sick leave of approx. one week. Rehabilitation and regeneration are more complex after a meniscus suture. After hospitalisation, which usually takes 4 days, the knee may only be partly stressed for about 6 weeks. The patient thus requires much longer sick leave of about 3 to 4 weeks. Normal sports activities are only possible after up to 6 months.

Depending on the severity, the treatment is either conservative, using physiotherapy, electrotherapy, and analgesics, or surgical.
Therapy for a meniscus rupture
In order to alleviate or completely eliminate pain and to restore the knee function, a meniscus rupture is treated conservatively or surgically, depending on the severity and the age of the patient.
Most meniscus ruptures require surgery. Surgery is necessary in the case of degenerative meniscal injuries of degrees 3 and 4, and for traumatic meniscal injuries (Becker et al. 2015). Depending on the type and size of the tear, either a meniscus suture or a partial meniscus removal is carried out. A meniscus suture means that the tear is sutured. In the case of a partial removal, the affected area is removed. In rare cases, the entire meniscus is removed and replaced with an implant. A meniscus suture and partial removal can also be used in combination in order to avoid having to remove too much of the natural meniscus (Müller-Rath & Ingenhoven 2011).
Apart from a few exceptional cases, meniscus surgeries are conducted arthroscopically. This involves making two small incisions on both sides of the knee, so that the procedure is minimally invasive. Surgery in this area is considered a routine intervention.
A purely conservative therapy includes physiotherapy and pharmacological treatment. It is used for smaller meniscal tears. Physiotherapy consists of a suitable treatment plan and movement therapy. If necessary, it may also include electrotherapy to prevent the degradation of supportive and protective leg muscles. Pain is treated mostly with cortisone-free medications. If the pain is severe, it can be treated with local anaesthetic injections or cortisone.
Rehabilitation of patients with a meniscus rupture
Rehabilitation is an extremely important phase after a meniscus rupture and is crucial for restoring the function of the entire knee. Extensive physiotherapy is essential, not only for conservative treatment of a meniscal tear, but also after surgery for more serious tears. The weakened knee must be slowly rebuilt through adapted training plans and physiotherapy. Additional electrotherapy may significantly accelerate the healing process.
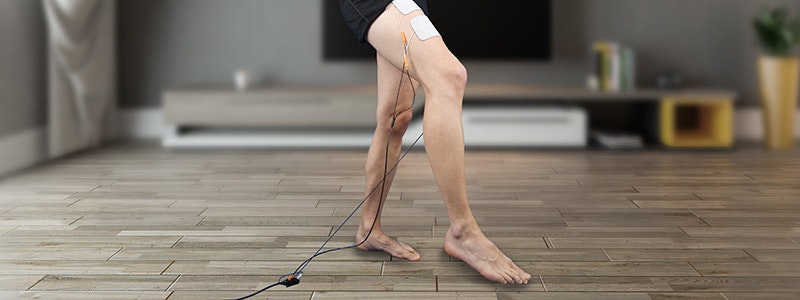
Functional electrical stimulation helps rebuild muscles after a meniscus rupture or surgery.
Electrotherapy
Electrical muscle stimulation may provide important support in every phase of rehabilitation, whether it involves treating pain with TENS programmes, or muscle strengthening. By selecting different programmes, the stabilising and protective muscles on the knee joint can be stimulated to prevent muscle atrophy (muscle wasting), which is caused by immobilisation after surgery of the menisci.
Stimulation of an isolated muscle with simple muscle strengthening programmes, or the combined stimulation of several muscles in a specific motion sequence through functional electrical stimulation. During the EMG-triggered electrical stimulation, the patient must actively tense the muscle. The electrical stimulation takes place once a predetermined activity threshold has been reached. The muscle is stimulated by the slowly increasing current with the pre-set intensity. Then the current is slowly decreased. This strengthens the thigh and is gentle on the knee.
Thorough rehabilitation is essential for the recovery of a meniscal tear. Physiotherapy is necessary regardless of the type or cause of the injury. The healing process can be even more effective when the treatment is combined with electrotherapy.
If you are a physician or therapist and are interested in further training in functional electrical stimulation or would like to organise STIWELL® training in your institute, please contact us
Prevention of a meniscus rupture
It is generally difficult to prevent a meniscus rupture. Injuries of this kind are mainly caused by a pathological load distribution or overloading and injuries caused by sports that put a lot of strain on the knee, such as football, handball, tennis, or skiing. Avoiding these sports, or a very thorough warm-up phase, may help reduce the risk of meniscus tears. Sports that are gentle on the joints, such as swimming or cycling, are good alternatives.
Reducing obesity may also serve as a preventative measure. It is particularly urgent if there is a leg malalignment (knock knees or bow legs).
The strain on the menisci can also be relieved by regularly changing one’s sitting position at the workplace.
Find out how functional electrical stimulation with the STIWELL® can be used to treat a meniscus rupture.
Becker, R., Buchner, M., Förster, J., Frosch, K. H., Losch, A., Niemeyer, P., Scheffler, S. & Siebert, C. H. (2015). S2k-Leitlinie der Deutschen Gesellschaft für Orthopädie und Unfallchirurgie: Meniskuserkrankung.
Müller-Rath, R., & Ingenhoven, E. (2011). Meniskusteilresektion. Arthroskopie, 24(1), 15-21.
Ruchholtz, S. & Wirtz, D. C. (2013). Orthopädie und Unfallchirurgie - essentials: Intensivkurs zur Weiterbildung. (2.Aufl.). Stuttgart: Georg Thieme Verlag.
Waldt, S. (2013). Meniskus-Update. Radiologie up2date, 13(04), 285-304.

