Traumatic brain injury (TBI)
A traumatic brain injury is an injury to the brain tissue due to an external impact on the skull, for example, due to accidents or falls.
Depending on the severity, a distinction is made between a concussion (mild TBI), a cerebral contusion (moderate TBI), and a brain compression (severe TBI). The therapy and rehabilitation depend on the severity of the trauma, and the nature and impact of the injury.
What is TBI and what treatment or therapy methods are available? Definition, numbers, causes, and diagnosis at a glance ...
What is traumatic brain injury?
TBI (ICD code: S06, T90.5) or ‘Traumatic Brain Injury’ (TBI) means damage to the brain caused by external trauma. The damage may occur indirectly, i.e. due to subdural, epidural, or intracerebral haemorrhage or oedema (swelling) caused by the trauma. In this case, the scalp, the skull, and the meninges (dura mater) remain intact. This injury is called a closed-head TBI.
Direct trauma usually causes damage to the scalp, the skull, and/or the meninges. This is called an open TBI.

Depending on how severely the brain is affected by the injury, it is possible to distinguish the following degrees of severity:
- Grade 1 TBI or commotio cerebri
It is often referred to as ‘concussion’ or ‘mild traumatic brain injury’. The consciousness of affected persons is usually not disturbed, or is only mildly disturbed (alert and oriented to somnolent; Glasgow Coma Scale (GCS) 13-15 points)
- Grade 2 TBI or contusio cerebri
It is often referred to as ‘cerebral contusion’ or ‘moderate traumatic brain injury’. The consciousness of affected persons is usually mildly to moderately disturbed (somnolent to soporific; GCS 9-12 points)
- Grade 3 TBI or compressio cerebri
It is often referred to as ‘brain compression’ or ‘severe traumatic brain injury’. The consciousness of affected persons is usually severely disturbed (comatose; GCS 3-8 points)
TBI occurs at a frequency of 150-300 per 100,000 inhabitants, with 30% of affected persons being under 30 years of age. 85% suffer from a mild TBI, 10% from a moderate TBI, and 5% from a severe TBI.
Symptoms of a traumatic brain injury
As is the case with any injury to the brain, TBI causes an immediate headache and nausea. It may also cause dizziness and vomiting. The symptoms that are initially observed include the following:
- Clouding of consciousness
The consciousness of the affected person may be mildly to strongly clouded. It may be easy, difficult, or impossible to wake them up (somnolence, sopor, or coma). - Low blood pressure (hypotension)
- Low or irregular heartbeat (bradycardia or arrhythmia)
- Irregular breathing
- Paralysis (paresis) or involuntary movements (bending or stretching synergies)
More accurate neurological examinations may reveal different symptoms, depending on the location and extent of the injury (similar to a stroke ):
- Numbness on one side (sensory disorder)
- Hemispatial neglect
- Language or speech disorders (aphasia or dysarthria)
- Difficulty swallowing (dysphagia)
- Balance or coordination disorders
- Visual impairment: defects of the field of vision (hemianopsias), double vision, etc.
- Cognitive impairment: numeracy disorders (dyscalculia), perception disorders, memory lapses (retrograde amnesia), etc.
Cardinal symptoms of a traumatic brain injury include headaches, nausea, and disorientation. Depending on the location and extent of the injury, there may also be different symptoms associated with movement, sensation, and/or cognitive functions.
Causes of traumatic brain injury
A TBI is usually caused by an accident. Common causes are falls, car or sports accidents. Particularly contact sports, such as ice hockey, boxing, or American football, pose a high risk for brain injuries. In these sports, the greatest risk is caused by repeated, minor brain injuries, which are not given enough time to heal.
Repeated trauma results in chronic traumatic encephalopathy, also known as boxer's encephalopathy. Increased awareness of this issue has led to the introduction of ‘concussion protocols’ in global professional sports leagues (NFL, NHL, NBA,
etc.).

Depending on the type of accident, there are different forms of brain damage:
- Coup/contrecoup
A severe trauma that makes the head move and then stop suddenly causes damage not only to the site of impact (coup), but also to the opposite side (contrecoup) due to the brain inertia.
- Direct damage to the brain stem
The brain stem is damaged by a displacement of the brain mass, which is caused by trauma to the lower jaw and hyperextension of the cervical spine.
- Diffuse axonal injury (DAI)
DAI is caused by the head hitting soft surfaces (e.g. in a car accident), especially in combination with rotational and acceleration forces. This results in the brain twisting within itself. This causes many small lesions and tears to the nerves (axons) throughout the brain (diffuse).
- Supratentorial mass displacement & herniation
Bleeding (subdural haematoma, epidural haematoma, intracerebral haematoma) or diffuse cerebral oedema (swelling) in the cerebrum may cause an entrapment (herniation) of brain tissue (at the tentorium or the foramen magnum) due to the downward shift of the brain mass.
Diagnosis: traumatic brain injury
Depending on its severity, TBI may be life-threatening. Immediate action is thus required. Emergency services should be notified immediately! If the affected person is conscious, he/she should be laid down, with their upper body positioned at 30°. If the affected person is unconscious, he/she should be placed in the recovery position.
If the patient is in medical care, the following examinations are usually carried out:
- Initial assessment & Glasgow Coma Scale (GCS)
The level of consciousness, the breathing, and the eyes (pupil size, reaction to light, optomotor response, etc.) are evaluated first.
The Glasgow Coma Scale is then used. It evaluates the opening of the eyes (1-4 points), the best verbal response (1-5 points), and the best motor response (1-6 points). A high score indicates no impairment, while a low score indicates a severe impairment.
- Clinical neurological examination
A closer examination focuses on the various symptoms that may also occur depending on the place of injury and extent. Such symptoms may involve swallowing, vision, or sensation.
- Imaging techniques
- Skull and cervical spine x-ray in suspected cranial or vertebral fracture
- Computed tomography (CT) and/or magnetic resonance imaging (MRI) to show the brain and the area of damage
- Additional examinations
- Electroencephalogram (EEG) in the event of epileptic seizures
- Evoked potentials (EVP) for measuring nerve conduction velocity
- Lumbar puncture in the case of suspected encephalitis (inflammation of the brain)
As a rule, the patient is admitted for at least 12-24 hours for observation, even with a mild TBI. In more severe cases, it is often necessary to admit the patient to an intensive care unit.
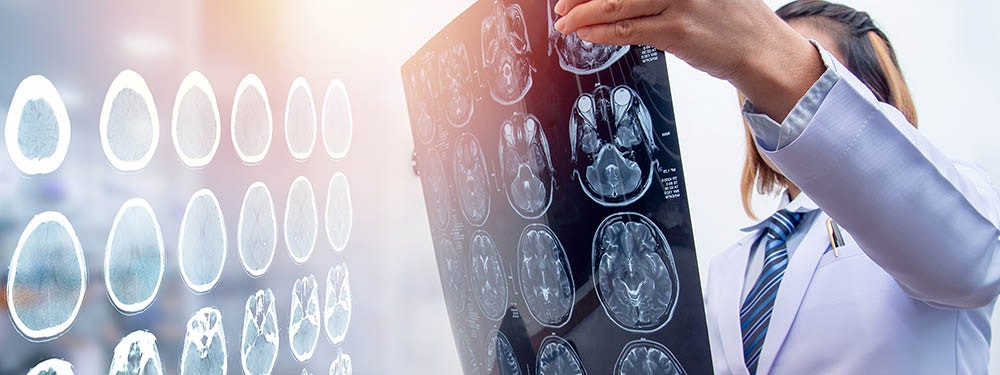
Imaging techniques such as CT or MRI are used to diagnose a potential traumatic brain injury..
Progression of a traumatic brain injury
A grade 1 TBI usually does not cause lasting neurological symptoms. Nausea and headaches may persist for several days or weeks (post-concussion syndrome). Grades 2 and 3 TBI, on the other hand, require treatment (treatment of traumatic brain injury) as well as targeted rehabilitation.
The trauma causes injuries to nerves and vessels in the brain, which result in bleeding and diffuse swelling. The space inside the rigid skull bone is limited, and the increase in volume causes increased pressure. The increased pressure may in turn cause damage or entrapment (herniations), which may even be life-threatening. Post-traumatic changes in cell metabolism may lead to further destruction of brain tissue, or secondary brain damage.
In severe cases, especially if there is diffuse damage and the midbrain is involved, the affected persons do not wake up from the coma (apallic syndrome). A TBI may even be fatal for polytrauma patients whose GCS score is initially low. TBI is considered the most common cause of death before the age of 40.
Due to the brain damage, spasticity (increased muscle tension) develops later on from paralyses (pareses). The damaged brain tissue may also trigger epilepsy, which can, however, be easily treated with medication. Personality changes may also occur due to brain damage.
Treatment of traumatic brain injury
The treatment of traumatic brain injury depends on its severity. In the case of grade 1 damage, headaches are the main complaint. They can be treated symptomatically by administering painkillers. Temporary bed rest (1 to 2 days) is also recommended.
In the case of serious damage (grades 2 and 3) with impaired alertness and breathing, the patient usually needs to be admitted to an intensive care unit. The usual treatments administered in an ICU include tranquillisers (sedation), fluid substitution, and monitoring of blood pressure, intracranial pressure, and blood circulation in the brain (cerebral perfusion pressure). Intubation and artificial respiration may also be required in some cases.
Surgery is usually required if there is a massive increase in intracranial pressure caused by severe swelling. Its aim is to obtain temporary pressure relief. This can be done by surgical opening of the skull (craniotomy) or drainage (draining fluid from the brain).
Other injuries that frequently occur during an accident, such as fractures, can be treated once the affected person is in a stable condition.
The treatment of traumatic brain injury depends on its severity. Various actions may be required, from bed rest to intubation with artificial respiration.
Rehabilitation after traumatic brain injury
In the case of concussion (grade 1), it is recommended to gradually resume activities following the period of bed rest. Especially in the case of sports accidents, attention must be paid to a slow reintegration into the training routine, and a provisional ‘contact ban’ (bodycheck, tackling, etc.).
In the case of cerebral contusion (grade 2) and brain compression (grade 3), the patient should be already regularly mobilised in the intensive care unit, even though his or her consciousness is impaired. With increasing alertness, initial standing and walking attempts can be carried out, and the breathing tube can be removed (extubation).Physiotherapy, occupational therapy & speech therapy
Specific therapeutic measures must be taken depending on the symptoms. Swallowing, language or speech disorders are treated by speech therapists. Movement disorders, which are usually caused by paralyses, are treated by physiotherapists. Cognitive impairments, such as numeracy or perception disorders, are diagnosed and treated jointly by neuropsychologists and occupational therapists.
More complex symptoms, such as hemispatial neglect or apraxia (difficulty with the planning or performing of movements), require an interdisciplinary approach, since they affect all activities of the affected person.
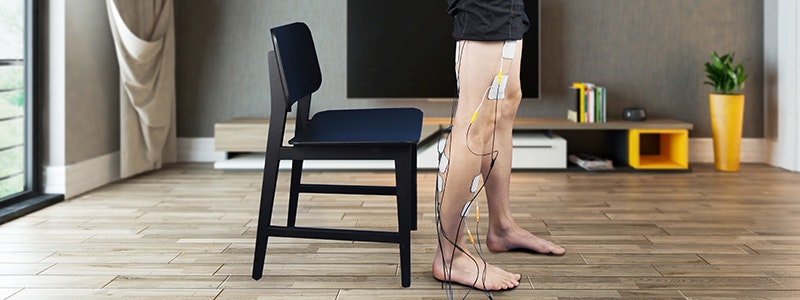
Functional electrical stimulation can be used to re-learn routine movements after a traumatic brain injury.
Electrotherapy
Functional electrical stimulation is a perfect supplement to rehabilitation for patients with TBI. Electrical stimulation can even be used in inpatient rehabilitation to counteract muscle paralysis. The aim is to use EMG-triggered electrical stimulation, where the patient begins the movement, and the current device amplifies the too weak impulse.
Multi-channel stimulation can enable everyday movements, such as standing up or grasping a glass. Frequent repetition can accelerate motor re-learning (Lang et al. 2007, 2009; Hauptmann & Müller 2011), and support integration into a normal everyday life.
Functional electrical stimulation can also enhance treatment with botulinum toxin (Botox) for spasticity (Hesse et al. 2005; Cotoi et al. 2018).
Outpatient treatment is necessary in most cases, even after discharge from the inpatient care. Daily training sessions for 30-45 minutes would be desirable (Platz 2011). However, outpatient treatment sessions are usually limited to 2-3 times per week. Electrical stimulation can increase the therapy frequency through targeted home-based therapy in order to achieve optimal results.If you are interested in continuing education on functional electrical stimulation and wish for a STIWELL® training directly at your institute or online, please contact us
Find out how electrical stimulation with the STIWELL® can be used in the treatment of a traumatic brain injury.
Cotoi, A., Iliescu, A., Foley, N., Mirkowski, M., Harris, J., Dukelow, S., Knutson, J., Chae, J., Miller, T., Lee, A., Janssen, S. & Teasell, R. (2018). EBRSR Evidence-Based Review of Stroke Rehabilitation. Chapter 10. Upper Extremity Interventions, 91.
Hauptmann, B. & Müller, C. (2011). Motorisches Lernen und repetitives Training. In: Nowak, D. (Hrsg.) Handfunktionsstörungen in der Neurologie. Berlin Heidelberg: Springer Verlag, 214-223.
Hesse, S., Werner, C., Pohl, M., Rueckriem, S., Mehrholz, J. & Lingnau, M. (2005). Computerized Arm Training Improves the Motor Control of the Severely Affected Arm After Stroke. A Single-Blinded Randomized Trial in Two Centers. Stroke, 36, 1960-1966.
Lang, C. E., MacDonald, J. R., & Gnip, C. (2007). Counting repetitions: an observational study of outpatient therapy for people with hemiparesis post-stroke. Journal of Neurologic Physical Therapy, 31(1), 3-10.
Lang, C. E., MacDonald, J. R., Reisman, D. S., Boyd, L., Kimberley, T. J., Schindler-Ivens, S. M., ... & Scheets, P. L. (2009). Observation of amounts of movement practice provided during stroke rehabilitation. Archives of physical medicine and rehabilitation, 90(10), 1692-1698.
Platz, T. (2011). Rehabilitative Therapie bei Armlähmungen nach einem Schlaganfall. Patientenversion der Deutschen Gesellschaft für Neurorehabilitation. Bad Honnef: Hippocampus Verlag.

