Cerebral palsy
Infantile cerebral palsy (ICP), also known as cerebral palsy, is an umbrella term for any brain damage that occurs in the womb or in infancy and causes motor disorders (movement).
What causes infantile cerebral palsy? What are the effects and which treatment or therapy methods are available? Definition, numbers, and diagnosis at a glance ...
What is infantile cerebral palsy?
Infantile cerebral palsy (ICD code: G80.-) is damage to the brain in the womb or in infancy (< 2 years). It is associated with lasting limitations. Cerebral palsy is thus a non-progressive developmental disorder of the immature, developing brain and is the main cause of childhood disability.
Symptoms vary depending on the location, extent, and cause of damage in the brain (lat. cerebrum). The affected children usually show a paresis (paralysis) of the limbs, i.e. the arms and/or legs, hence the term infantile cerebral palsy.
Since ICP is a clinical diagnosis and symptoms are still only developing, the full clinical presentation often only becomes apparent later in life, even though the damage occurs before or immediately after birth. Brain lesion usually occurs in the 3rd trimester (29-40th week of pregnancy), and the diagnosis is made between the first and second year of life. If symptoms are not pronounced, a diagnosis is often made later.
ICP affects approx. 2 out of every 1000 newborns. Premature babies and babies with a low weight at birth are more likely to be affected. Periventricular leukomalacia (damage to the white matter in the brain) is also a risk factor for ICP.

The symptomatic treatment, especially in children who are severely affected, should start as soon as possible. Interdisciplinary collaboration between different departments and adequate school care are of particular importance.
Synonyms of infantile cerebral palsy
The current term ICP has various synonyms:
CP disease, ICP disease, early childhood brain damage, infantile brain damage, cerebral palsy, infantile paralysis, cerebral movement disorder, cerebral dysfunction, etc.
The following terms are now obsolete:Little’s Disease, Foerster's syndrome/diplegia
Causes - What causes ICP?
The causes of ICP are diverse. Various prenatal, perinatal, and neonatal events (before, during, and after birth) may damage the brain, either on their own or in combination with other factors. However, no cerebral cause can be found in about 20% of ICP cases.
For a long time, it was assumed that asphyxia (lack of oxygen during birth) was the main cause of ICP. We currently know that prenatal factors play a greater role, and that problems during childbirth are responsible for only about 20% of ICP cases.
The impairments vary depending on the developmental stage of the child at which the disorder occurred. The basic structure of the brain develops before the 24th week of pregnancy, and disorders that occur during that time cause malformations. It is only
after that period (3rd trimester) that damage to the brain tissue occurs.
Prenatal risk factors
- Genetics (gene mutations, etc.)
- Viral or bacterial infections: Rubella, toxoplasmosis, chorioamnionitis (bacterial infection of the foetal membranes), etc.
- Medicines, alcohol, drugs
- Infarcts or cerebral haemorrhage (periventricular leukomalacia, intraventricular/periventricular haemorrhage, infarcts of large cerebral arteries - middle cerebral artery, etc.)
Perinatal risk factors
- pH value of the umbilical artery
- Complicated childbirth: oxygen deficiency (Apgar score <4) and brain haemorrhage
Neonatal risk factors
- Vascular injury (periventricular leukomalacia, intraventricular/periventricular haemorrhages)
- Oxygen deficiency (apnea syndrome)
- Neonatal seizures
- Severe blood poisoning (sepsis)
- Hydrocephaly (posthaemorrhagic hydrocephalus)
- Meningitis
- Severe neonatal jaundice
Childhood brain damage may have various causes, such as infections, lack of oxygen, bleeding, or infarction. However, it is not always possible to find a cerebral cause.
Symptoms of infantile cerebral palsy
Brain damage in infants with ICP causes impaired movement (upper motor neuron). Depending on the damage location, a (spastic) paresis may affect the arms, the legs, the torso, or the face. Damage affecting the cerebellum or the basal nuclei may also cause
coordination disorders or muscle tone disorders (ataxia, dyskinesia, athetosis, etc.). Similar to
a stroke, there may be different symptoms, depending on the location and extent of the damage.
The following symptoms are characteristic for infantile cerebral palsy:
Spastic paralysis (paresis)
Spasticity means pathologically increased muscular tension, which is usually accompanied by stiffness (contractures). It is caused by damage to the brain (upper motor neuron), and manifests itself in the form of spastic paralysis (paresis). Pareses may take various forms, depending on the location and the extent of damage:
- Monoparesis
Spastic paralysis affects only one limb (usually one leg). - Paraparesis
Spastic paralysis affects the legs; the arm function is normal. - Hemiparesis
Spastic paralysis affects one arm and one leg on one side of the body (may affect predominantly one arm or one leg). - Triparesis
Spastic paralysis affects one arm and both legs (combined hemiparesis and paraparesis). - Diparesis
Spastic paralysis affects the arms and legs, while the legs are usually more affected. - Tetraparesis
Spastic paralysis affects the arms and legs, and control over the torso and head is impaired. - Bilateral hemiparesis
Spastic paralysis affects the arms and legs, while the arms are usually more affected.
If spasticity occurs in ICP, it is called unilateral or bilateral spastic cerebral palsy. For bilateral paresis, a distinction is made between a symmetrical and an asymmetric distribution pattern (Döderlein 2015).

Brain damage in ICP leads to impaired movement (1st motoneuron). Depending on the location of the damage, (spastic) paresis of the arms, legs, trunk or face occurs.
Athetosis
Athetosis refers to a movement disorder (hyperkinesia/excessive movement), which causes slow, involuntary, and convoluted movements. The reason for these movements is a coordination disorder between the agonist and antagonist muscles, with constantly changing muscle tension.
Since these excessive movements occur mainly in the face and in neck muscles, they often give the unjustified impression of an intellectual disability.
Ataxia/hypotension
Ataxia is a coordination disorder. Ataxia in the arms causes erratic, jerky movements with a poor aim. Ataxia in the lower limbs or the torso causes impaired balance, gait disorders and static ataxia. It is often combined with a low basic tone of the muscles (hypotonus).
There are different forms of ICP, depending on the symptoms. Since the symptoms may also occur in combination, common symptom complexes are grouped together as syndromes (forms and syndromes).
Additional impairments/concomitant symptoms of ICP
In addition to movement disorders, brain damage may cause other symptoms or concomitant diseases:
- Sensory processing disorder
Sensory deficits (tactile and proprioception, pain sensation), impaired vision, hearing disorders - Disorders of spatial and body perception (perception)
- Communication impairment
with regards to language, speech and speech comprehension - Impaired oral functions
Uncontrolled salivation, difficulty in swallowing (which may be caused by malnutrition and aspiration with subsequent pneumonia), etc. - Vegetative and hormonal disorders
Disorders of bladder and bowel function, circulation, heat and cold adaptation, sweating, etc. - Reduced bone density
Bone fractures are more likely - Epilepsy
Seizures are common concomitant symptoms, especially for patients with hemiplegia and quadriplegia (tetraplegia) - Behavioural issues
Cognitive deficits, drive disorders, psychological disorders, etc.

The main symptoms of infantile cerebral palsy are spastic paralysis, athetosis (excessive movements), and/or ataxia (coordination disorder).
Forms & syndromes of infantile cerebral palsy
Depending on the relevant symptoms, ICP may take different forms or syndromes:
- Spastic cerebral palsy
- Spastic diparesis syndrome
- Spastic hemiparesis syndrome
- Tetraparesis syndrome
- Athetoid cerebral palsy (with athetosis as the main symptom)
- Ataxic cerebral palsy (congenital ataxia syndrome)
- Mixed cerebral palsy
Spastic cerebral palsy is the most common form at 70%-80%. The athetoid (8-20%) and ataxic (5%) forms of ICP, on the other hand, are less common (von Loh 2017). Mixed forms of ICP, in which two of the main symptoms occur in combination, are also common. In most cases, there is a combination of a spastic and an athetic disorder. Intellectual disabilities are more likely to occur in patients with these mixed forms.
Progression & prognosis of infantile cerebral palsy
The prognosis depends heavily on the severity, the concomitant symptoms, and the form of the cerebral palsy. With appropriate treatment, children who are mildly affected may be able to lead a normal life with few restrictions.
The inclusion of these children in regular school life remains a big problem. Many teachers or schools are unwilling to accept children with physical disabilities, even if they are not intellectually impaired. Some children with infantile cerebral palsy, however, may learn slower, or may have more difficulties due to cognitive or linguistic limitations. Individual early intervention is of central importance here.
Limited motor skills (spasticity, ataxia, etc.) may cause difficulty walking and grasping. As a result, walking aids, sometimes even a wheelchair, may be necessary, and self care (dressing, washing, eating, drinking, etc.) may be impaired.
Movement disorders affect the joints, bones, and muscles of the growing child. They may cause contractures (rigidity), reduced growth, or deformities (deformations). Deformities, for example, in the spine (scoliosis), in the femur (coxa valga), or equinus are also common. Spasticity in the adductors of the hip joint causes an increased risk of hip dislocation.
The life expectancy of children who are severely affected may be shortened due to a number of additional risk factors (aspiration/pneumonia), especially if they suffer from dysphagia.Diagnosis: infantile cerebral palsy
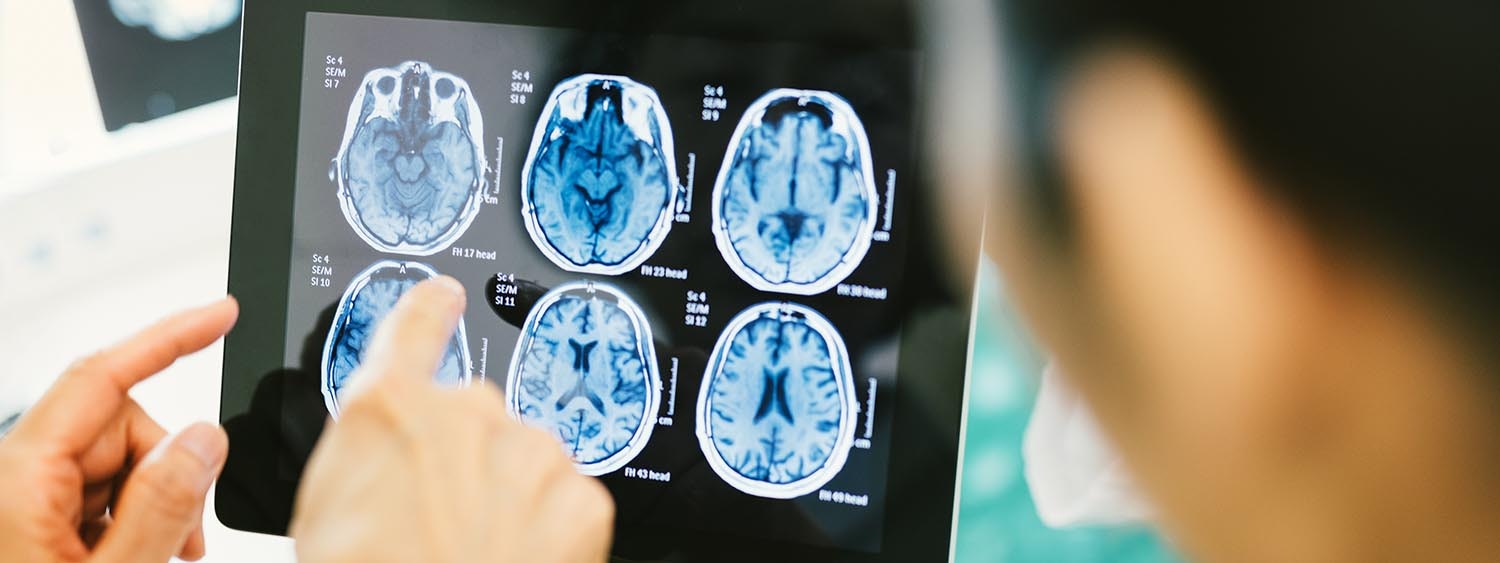
The diagnosis is made in the first or second year of life on the basis of the clinical symptoms and, if necessary, in combination with diagnostic imaging techniques and other additional examinations..
ICP is a clinical diagnosis, i.e. it is based on the symptoms. Even if the injury is prenatal, perinatal, or neonatal, the clinical presentation of ICP often develops later in life. Thus the diagnosis is usually made only in the second year of life, or, in particularly mild cases, even in the fourth or fifth year of life.
Diagnostic imaging of the brain, usually an MRI (magnetic resonance imaging) scan, is also performed. Blood tests and special tests to assess nerves and muscles (nerve conduction velocity test, electromyography, etc.) or genetic tests may also provide more information.
Severity assessment
Once the diagnosis has been made, motor limitations are evaluated to assess the degree of severity. This assessment is particularly important, on the one hand, to document the patient’s current state of health and, on the other hand, to document the progression. Various scores are available to assess the severity of ICP symptoms.
The most common classification is the ‘Gross Motor Function Classification System’ (GMFCS) because it is based heavily on the WHO international classification of functionality, disability, and health (ICF). The GMFCS has different levels:
- GMFCS level I
Patients can walk and climb stairs without the use of a banister. Running and jumping, however, are limited. There is a mild balance and coordination impairment. - GMFCS level II
Patients are able to walk, but may experience difficulty balancing on uneven terrain and inclines. They have to use the banister when climbing stairs. Running and jumping are more limited. - GMFCS level III
Patients walk using walking aids in indoor and outdoor settings. They require support or wheelchairs when travelling longer distances. - GMFCS level IV
Patients may be able to change position with minimal help. Walking is very limited. They mostly use wheelchairs every day. - GMFCS level V
Voluntary motor function is hardly present; extensive aids are required for standing and sitting; independent mobility may be retained using electric wheelchairs.
Therapy of infantile cerebral palsy
Cerebral palsy is caused by a single instance of damage to the brain that occurred previously (e.g. infarction). This damage cannot be remedied afterwards, which makes causal therapy impossible. Even preventive treatment is currently impossible due to the diverse or sometimes inexplicable genesis of ICP.
The treatment of ICP is solely symptomatic. The focus is on treating movement disorders. Medications are used to improve symptoms, such as coordination and tone disorders. Spasticity, which is very common, can not only be treated with medications (baclofen, etc.), but also with local injections (botulinum toxin). Psychological symptoms or epilepsy can be improved in most cases by targeted pharmacological treatment.
Changes in the skeletal system, especially deformities, require orthopaedic interventions. If necessary, splints or even surgery may be required to avoid secondary complications.

Early intervention programs to support children with cerebral palsy
Treatment of infantile cerebral palsy
Symptomatic therapy is at the heart of treatment of children with ICP. Depending on the severity of the symptoms, it may be useful to contact a specialised support organisation, or arrange for outpatient physiotherapy, occupational therapy, speech therapy, and electrical stimulation.
Early intervention
It is important to seek help from specialised institutions that offer early intervention programmes, especially for children with cognitive impairments. The programmes are adapted to the needs of the child, and children are supported in all aspects of life. Physiotherapy, occupational therapy, and speech therapy are part of the daily schedule, as are support at school and help with daily routine tasks (personal care, eating, self-sufficiency, etc.).
Support organisations are available from kindergarten age via the usual school age up to the age of 18. There are various models in which it is possible to attend special education classes, or to take advantage of day care - also in combination with assisted living services (all-seasons care). Young adults are often offered vocational training.
Physiotherapy, occupational therapy & speech therapy
All motor function disorders (movement) and speech disorders are treated by different disciplines (physiotherapy, occupational therapy, and speech therapy). Especially in the case of children, an individual, child-centred, shared goal in therapy is essential to achieve success. In order to achieve this, intensive interdisciplinary cooperation between therapists is required.

Functional electrical stimulation in infantile cerebral palsy
Electrotherapy
Functional electrical stimulation (FES) is establishing itself as an integral part of the motor learning process in the treatment of children. Children tolerate it very well, and it improves the performance of actions that are suitable for children (Bosques et al. 2016).
For motor learning, the context of the activity that is being trained using EMG-triggered multi-channel electrical stimulation (EMG MES) is of particular importance. Multi-channel electrical stimulation is especially beneficial for children with cognitive impairments, or those who have problems with exercise programmes (Chiu, HC, & Ada, L. (2014). The variety of stimulation channels facilitates complex movements, and thus activity-related actions.
FES can be used to achieve various goals:
- independence in everyday life (e.g. eating, playing)
- improved walking ability
- reduced muscle tension (spasticity)
- improved mobility
- increased muscle strength and improved coordination
If you are interested in continuing education on functional electrical stimulation and wish for a STIWELL® training directly at your institute or online, please contact us
Find out how functional electrical stimulation with the STIWELL®
can be used in the treatment of infantile cerebral palsy.
Bosques, G., Martin, R., McGee, L., & Sadowsky, C. (2016). Does therapeutic electrical stimulation improve function in children with disabilities? A comprehensive literature review. Journal of pediatric rehabilitation medicine, 9(2), 83-99.
Chiu, H. C., & Ada, L. (2014). Effect of functional electrical stimulation on activity in children with cerebral palsy: a systematic review. Pediatric Physical Therapy, 26(3), 283-288.
Döderlein, L. (2015). Infantile Zerebralparese: Diagnostik, konservative und operative Therapie. (2. Aufl.). Berlin Heidelberg: Springer Verlag.
Von Loh, S. (2017). Entwicklungsstörungen bei Kindern: medizinisches Grundwissen für pädagogische und therapeutische Berufe. Kohlhammer Verlag.

