Drop foot
Drop foot means a loss of strength in muscles that lift the foot. It is caused by nerve damage. This damage may occur in the brain, the spinal cord, or the leg.
Which muscles are affected by drop foot? What treatment or therapy methods are available? Definition, causes, and progression at a glance...
What is a drop foot?
Drop foot is a symptom. It describes the limited possibility of lifting the foot due to reduced strength in one or more of the following muscles:
- anterior tibial muscle (tibialis anterior muscle)
- fibularis muscle (longus/brevis)
- toe lifter (extensor digitorum longus muscle)
- big toe lifter (extensor hallucis muscle)
Drop foot is particularly noticeable during heel-to-toe walking and when the leg swings forward when walking. Forefoot, toes and/or the edge of the foot are not lifted sufficiently, or cannot be lifted at all (foot drop). This changes the gait pattern. The leg/knee must be raised further so that the affected foot does not get caught on the floor (stair-climbing movement). There may also be other changes in the gait pattern to avoid falls due to the foot getting stuck.
The gait disorder causes poor posture and pain over time, which is why early treatment is recommended. Drop foot can be caused by damage to the central nervous system (upper motor neuron: in the brain or spinal cord), or the peripheral nervous system (lower motor neuron: from the spinal cord to the muscle).
Drop foot due to peripheral damage is also called peroneal nerve palsy or peroneal nerve paralysis . This means damage to the peroneal nerve, which is also known as the fibular nerve. Peripheral damage causes flaccid paralysis, i.e. an isolated paresis of muscles that lift the forefoot, whereas central damage causes spastic paresis, i.e. a combination of calf spasticity and paresis of the forefoot lifting muscles.

Drop foot not only affects walking, but also climbing stairs.
Side note: lateral popliteal nerve
The common peroneal nerve, also known as the common fibular nerve, originates from the sciatic nerve and divides into the superficial fibular nerve (superficial peroneal nerve) and the deep fibular nerve in the knee area. The superficial fibular nerve supplies the area of the skin from the lower leg to the back of the foot as well as the fibularis (peroneus) longus and brevis muscles, which lift the side of the foot. The deep peroneal nerve (nervus fibularis profundus) is responsible for lifting the feet and toes, and for sensation (feeling) in the area of skin between the first and the second toe.
Causes of drop foot
There are many reasons for a drop foot. Generally, a distinction is made between drop foot due to a progressive (chronic and progressive) underlying disease, or due to a stable (non-progressive) underlying disease in the central nervous system (brain or spinal cord) or peripheral nervous system (nerve fibularis).
They following may cause foot drop due to central damage:
- stroke
- multiple sclerosis
- traumatic brain injury
- cerebral palsy (early childhood brain damage)
- paraplegia , etc.
The following may cause foot drop due to peripheral nerve damage to the fibular nerve:
- fractures in the area of the knee or the lower leg with nerve involvement, etc.
- Baker's cyst (fluid collection in the area of the popliteal fossa)
- pressure damage due to staying in a certain position for too long (crossing the legs or incorrect positioning of the legs during bed rest)
- pressure damage due to cast treatment (plaster cast) following injuries to the bones
A herniated disc may also cause foot drop. In the event of a herniated disc, the gelatinous
core of the inner vertebral disc is pressed outwards. It may then pinch the peripheral nerve (nerve root) that leaves the spinal cord. Foot drop may also occur if the nerve is pinched in a certain area of the lumbar spine (L4, L5, S1), which primarily
supplies the fibular nerve.
Drop foot may also occur if the sciatic nerve is pinched.
Progression of drop foot
The weakness means that the muscles that were once supplied by the nerve lose strength and consequently decrease in mass (cross-section and number of myofilaments). Over time, fibrosis and adipose tissue replace the lost mass in the muscle.
Central damage, which causes spastic paresis, i.e. a combination of calf spasticity and paresis of the forefoot lifter, often results in contractures (stiffening of the joints) over time. As a result, the foot tends to adopt a splay foot position.

Strengthening exercises are particularly important for patients with drop foot in order to rebuild their muscles.
Therapy & treatment of drop foot
Depending on the cause of the paresis, various treatment options can be useful.
Generally, a physician must be consulted immediately in the case of a sudden onset of paralysis. The cause could be life-threatening, for example, a stroke. In this case, the underlying disease must be treated first. This usually results in an improvement of the symptom, i.e. the paresis. A sudden drop foot may also occur due to a herniated disc. Also in this case, it is necessary to consult a physician immediately. These cases usually require prompt surgery to prevent permanent damage to the nerve.
In most cases, however, the weakness progresses slowly, and the patients are aware of the cause. In this case, conservative, symptomatic treatment should be considered first. This could mean providing splints (foot orthoses), as well as physiotherapy. Surgery to correct the foot position, or a muscle transposition, should be considered only in very serious cases, for example, if a splay foot position has already developed.Physiotherapy
The therapy varies depending on the underlying disease. If the nerve damage has an orthopaedic cause, such as a herniated disc or wear of the knee joint, local treatments on the back or knee can be useful. These treatments could include manual techniques, as well as massage or stabilisation exercises. If there is a central neurological cause, such as a stroke, the therapy focuses on practical exercises.
Regardless of the cause, strengthening exercises for the weakened foot lifter muscle(s) and stretching exercises for the calf muscle should be started from the outset. With increasing muscle strength, gait training should be considered to restore a normal gait pattern. In most cases, pain caused by the gait disorder or poor posture must also be treated.
Functional electrical stimulation
EMG-triggered electrical stimulation can promote functional recovery and facilitate performing everyday activities. Electrical stimulation can strengthen the movement of weakened muscles in such a manner that movements such as getting up or walking, which were previously problematic, can be performed again. After consistent training, the success becomes apparent in everyday life, even without electrical stimulation.
Electrical stimulation is particularly important in the case of peripheral damage. Due to the injury, the muscle sections supplied by the nerve can no longer be moved voluntarily. Special currents (low frequency and long pulse duration) can maintain the muscle structure until the nerve has recovered.
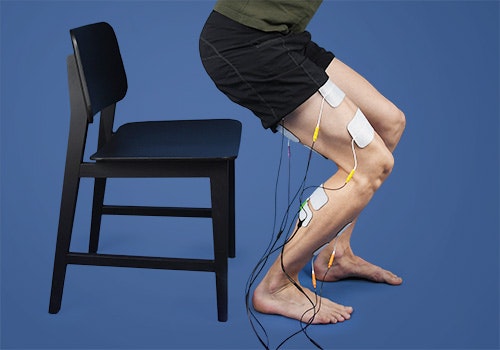
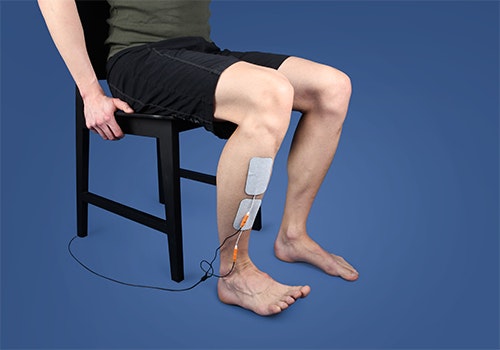
Functional electrical stimulation can be used to train everyday activities, such as getting up, for patients with drop foot.
If you are interested in continuing education on functional electrical stimulation and wish for a STIWELL® training directly at your institute or online, please contact us
Find out how functional electrical stimulation with the STIWELL® can be used to treat drop foot.

