Ataxia
Ataxia is a movement disorder that is primarily caused by impaired coordination. It may manifest itself in a variety of movements involving the arms, legs, and torso, but it is most frequently observed when standing, walking, or grasping.
What is ataxia? What treatment or therapy methods are available? Definition, forms, and causes at a glance ...
What is ataxia?
Ataxia is a form of movement disorder in which the coordination or fine-tuning of movements is impaired (Greek a-taxis = disorder.) An interaction between the cerebrum, cerebellum, brainstem, nerves, and muscles is important for a well-coordinated movement.
A malfunction in one of these components, e.g. in the cerebellum, causes uncontrolled, excessive, or erratic movements. Excessive movements may affect the entire body. There are different forms of ataxia, depending on where it occurs.
Ataxia may also manifest itself as eye movement disorders. It may cause involuntary eye movements (nystagmus), and/or impaired eye movement (e.g. slow smooth pursuit eye movement), as well as impaired backward eye movement (saccades).
Ataxia may also affect speech muscles, and thus lead to a speech disorder (dysarthria). Those affected usually have choppy speech and unusual intonation.
In all cases, intensive therapeutic care is particularly important in order to minimise the impact of ataxia on the patient’s daily routine and social life.

Ataxia impairs coordination, and thus purposeful movements that are often necessary in everyday life.
Forms of ataxia
There are various forms of ataxia, depending on which body parts are affected:
- Limb ataxia
This is a motor coordination disorder affecting the arms and/or legs (upper/lower limbs). It manifests itself in coarse and shaky movements. It is visible in arms and hands especially in the form of rapidly alternating movements (diadochokinesia) and in handwriting. Targeted movements, such as when grasping a glass, may miss the target (dysmetria). Atactic leg movements manifest themselves especially when standing and walking (see static/gait ataxia).
- Truncal ataxia
Truncal ataxia manifests itself as shaky, uncoordinated movements of the torso, which may even lead to a loss of balance. Truncal ataxia can be observed in the sitting position, especially when the patient’s feet hang freely and arms are stretched out in front of him or her.
- Static ataxia
Static ataxia is visible when standing and, similar to truncal ataxia, manifests itself in a systematic or unsystematic swaying of the body. The swaying may be so strong that the patient loses his or her balance and falls to the ground.
- Gait ataxia
Coordination disorders usually manifest themselves in an unsteady gait when walking. Those affected attempt to compensate by increasing their pace, stiffening their body, and/or holding on to objects or walls.
Causes & classification of ataxias
Ataxias can be classified according to the location of damage or the cause.
Depending on the location of damage, one refers to a disorder of the central nervous system (CNS) or of the peripheral nervous system (PNS). In the case of damage to the CNS, a distinction is made between a cerebellar ataxia and a spinal
(or sensory) ataxia. Cerebellar means that the cause lies in the cerebellum. Spinal means that the cause lies in the spinal cord. Disorders of peripheral nerves (PNS) are often caused by polyneuropathies.
However, the most common classification is by type of cause:
- Genetic or hereditary ataxias
Depending on the mode of inheritance, a distinction is made between autosomal (recessive or dominant) or x-linked cerebellar ataxias. Autosomal recessive forms, such as Friedreich's ataxia (FRDA), are characterised by their early onset (in childhood). Autosomal dominant forms, such as spinocerebellar ataxia (SCA), usually begin in adulthood.
- Acquired ataxias
The term acquired ataxias refers to all forms of non-congenital ataxia. It means all those forms that are caused by an injury. The cause may be, for example, a stroke, multiple sclerosis, a traumatic brain injury, cerebral haemorrhage, tumours, as well as alcoholic cerebellar degeneration (ACD) or paraneoplastic cerebellar degeneration (PCD: autoimmune disorder in the context of various tumours).
- Idiopathic or sporadic ataxia
It is not possible to establish either genetic or acquired causes, even though ataxia is clinically evident. This form is called an idiopathic or sporadic ataxia. This form includes, for example, the multiple system atrophy, cerebellar type (MSA-c).
A distinction is made between various forms of ataxia. They may have a variety of causes (such as a stroke)..
Diagnosis: ataxia
Detailed case history (medical history) and a neurological examination are necessary to diagnose ataxia. This is followed by a relevant imaging technique, usually magnetic resonance imaging (MRI). If a genetic cause is suspected, biochemical and molecular genetic laboratory diagnostics are carried out.
Various clinical scales can be used to measure the severity of different ataxia symptoms. The ‘International Cooperative Ataxia Rating Scale’ (ICARS) and the ‘Scale for Assessment and Rating of Ataxia’ (SARA) are used to assess symptoms of static ataxia, gait ataxia, limb ataxia, and speech ataxia. In the case of Friedreich's ataxia (FRDA), the clinical FRDA scale is used to assess the specific symptoms.
Therapy & treatment of ataxia
The cause of ataxia can be treated in acquired ataxias, if at all. Otherwise, the focus is on regular professional counselling and/or treatment. Rehabilitative measures, such as physiotherapy, occupational therapy or speech therapy, focus on active coordination support.
Functional electrical stimulation may support the coordination training. EMG-triggered multi-channel electrical stimulation supports practical coordinated movements in a natural way. The EMG measurement allows the affected person to initiate the movement independently. By using up to 4 stimulation channels, muscle coordination in several muscle groups can be improved in such a manner that a controlled movement can be performed and the re-learning of lost functions is accelerated.
Daily coordination training at home with short exercise sessions (about 20 min. each) is recommended for patients with ataxia in order to achieve optimal therapy results.
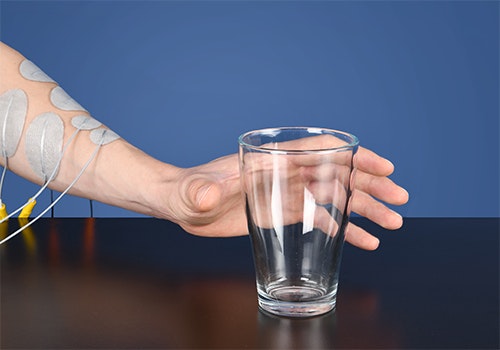
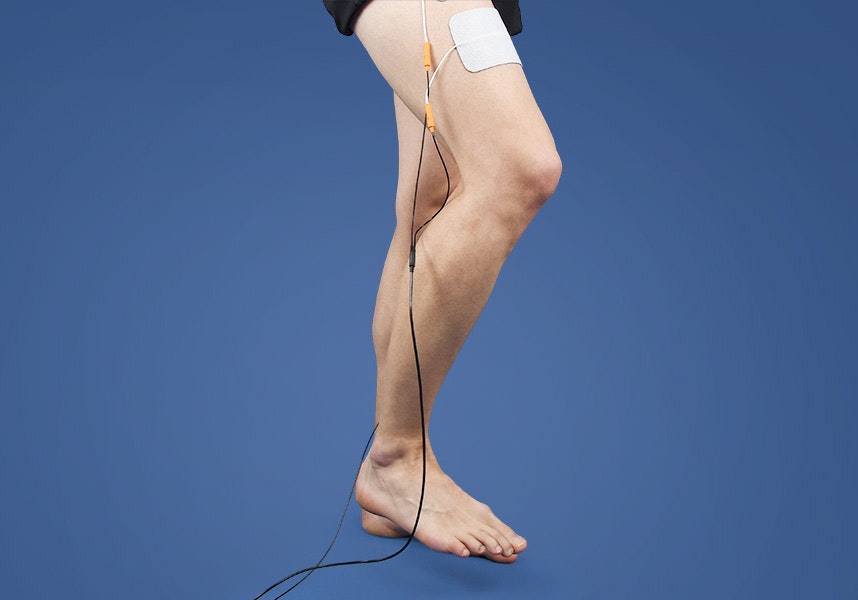
Functional electrical stimulation can be combined with everyday activities to improve coordination in patients with ataxia.
If you are interested in continuing education on functional electrical stimulation and wish for a STIWELL® training directly at your institute or online, please contact us
Find out how functional electrical stimulation with the STIWELL® can be used in the treatment of ataxia.

